By: Thomas Meinel, Peter Kelly and Alastair Webb
twitter: #GSSW @TotoMynell
ESO Garmisch Stroke Science Workshop 2021
Session 3: Stroke Recovery and Rehabilitation
With his keynote lecture “Dementia Prevention after Stroke,” Edo Richard from the Netherlands raised a topic of utmost importance to patients and caregivers. Multiple pathophysiological pathways including direct vascular damage, but also inflammation, neurodegeneration and hypoperfusion contribute to cognitive impairment. Currently available trials on this topic are limited by short follow-up, a focus on motor recovery and recruitment of patients mostly in the acute phase. There are also heterogeneous trajectories of cognition after stroke and this has to be taken into account for future trial design.
Blood pressure reduction seems to have a significant, but only very small effect on dementia prevention in vascular preventive trials. For stroke patients, however, there is no clear evidence for that and the sweet spot for target systolic blood pressure is to be determined. A U shaped relationship of blood pressure with dementia following stroke, particularly in the elderly, suggests the hypothesis that even de-prescribing antihypertensives might be an option for some patients. Blood pressure variability is also associated with dementia following stroke – calcium channel blockers might be the best drug when blood pressure variability is the major problem. Although 30-40% of dementia cases are due to modifiable risk factors, the circular reasoning that optimizing those risk factors can subsequently prevent those dementia cases may not be true and we should have realistic expectations about the possibilities to prevent post-stroke dementia.
The call for trialists and funders to take cognition into account and to run large trials with long-follow up periods was the start to a vivid discussion that covered controversies on de-prescription trials, and the addition of cognitive endpoints into stroke trials.
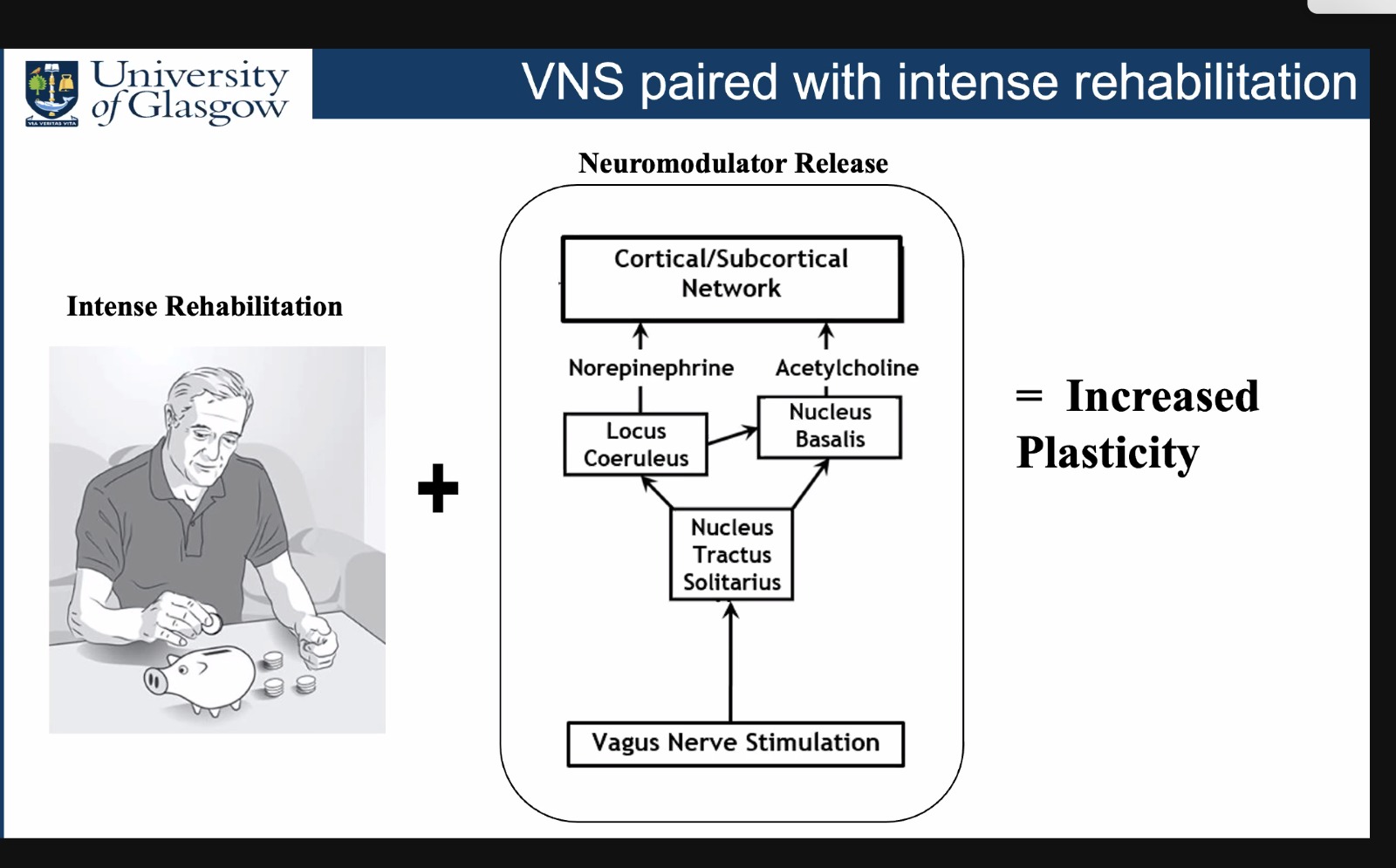
Jesse Dawson from the United Kingdom showed promising data on vagus nerve stimulation for motor recovery after stroke. He nicely explained the translational research history build on the hypothesis that vagus nerve stimulation could enhance plasticity in addition to intensive physical therapy, even in chronic stroke patients. That led to a positive trial in moderately affected chronic stroke patients and FDA approval of this therapy. The study had one serious safety event, namely one patient with a transient vocal cord paresis. In Europe, approval for this treatment option is pending.
How to use imaging biomarkers for recovery trials was the topic of Marco Düring from München and Basel. He nicely explained the drawbacks, but also opportunities of (imaging) biomarkers as a surrogate endpoint in clinical trials. Pitfalls include clinical validation (proof of principle and effectiveness), but also technical validation (repeatability and reproducibility) and other factors such as availability, cost and equipment validation. The main chance is to increase feasibility of trials by drastically reducing the sample size.
Lastly, Gillian Mead from the UK presented a synopsis on pharmacological and non-pharmacological treatment options for fatigue post-stroke. Up to 50% of stroke patients experience fatigue and it is more prevalent in women and depressed patients. The most important aspects to be addressed seem to include activity, mood, sleep quality, as well as negative thoughts and pain management. Serotonergic drugs had no effect on fatigue and trials on Modafinil, psychological therapy, cognitive and graded activity training and transcranial direct current stimulation are on the way.
The convenors Alastair Webb and Peter Kelly did a great job balancing the certainties and uncertainties of the data. The final energetic discussion followed the talks and covered insights into trial designs, pathophysiological explanations and the clinical application of the research.